Connect With Us
Blog
Blog
Types of Foot Arthritis
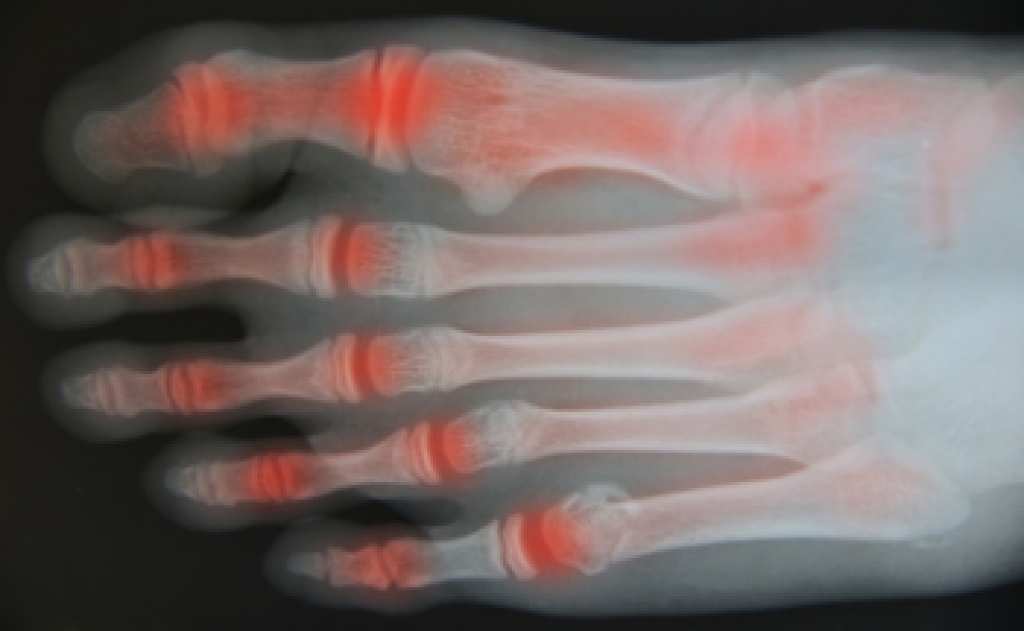
Arthritis in the feet causes inflammation and damage within the joints, leading to discomfort and reduced mobility. Several types can affect the feet, including osteoarthritis, which involves wear and tear of cartilage. Rheumatoid arthritis is an autoimmune condition that attacks joint lining. Psoriatic arthritis is linked to psoriasis, and gout is caused by crystal buildup in the joints, often affecting the big toe. Symptoms include pain, swelling, stiffness, and difficulty walking. Causes and risk factors include aging, joint injury, genetics, and underlying health conditions. Without proper care, symptoms can worsen over time. A podiatrist can evaluate the condition, provide treatment options, and recommend supportive footwear. If you have symptoms of arthritis in your feet, it is suggested that you consult a podiatrist who can offer effective relief and management tips.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Stephen Boykins, DPM from SoCal Podiatry, P.C.. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a term that is commonly used to describe joint pain. The condition itself can occur to anyone of any age, race, or gender, and there are over 100 types of it. Nevertheless, arthritis is more commonly found in women compared to men, and it is also more prevalent in those who are overweight. The causes of arthritis vary depending on which type of arthritis you have. Osteoarthritis for example, is often caused by injury, while rheumatoid arthritis is caused by a misdirected immune system.
Symptoms
- Swelling
- Pain
- Stiffness
- Decreased Range of Motion
Arthritic symptoms range in severity, and they may come and go. Some symptoms stay the same for several years but could potentially get worse with time. Severe cases of arthritis can prevent its sufferers from performing daily activities and make walking difficult.
Risk Factors
- Occupation – Occupations requiring repetitive knee movements have been linked to osteoarthritis
- Obesity – Excess weight can contribute to osteoarthritis development
- Infection – Microbial agents can infect the joints and trigger arthritis
- Joint Injuries – Damage to joints may lead to osteoarthritis
- Age – Risk increases with age
- Gender –Most types are more common in women
- Genetics – Arthritis can be hereditary
If you suspect your arthritis is affecting your feet, it is crucial that you see a podiatrist immediately. Your doctor will be able to address your specific case and help you decide which treatment method is best for you.
If you have any questions please feel free to contact our offices located in Downey and Moreno Valley, CA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Achilles Tendon Pain Can Affect Daily Movement
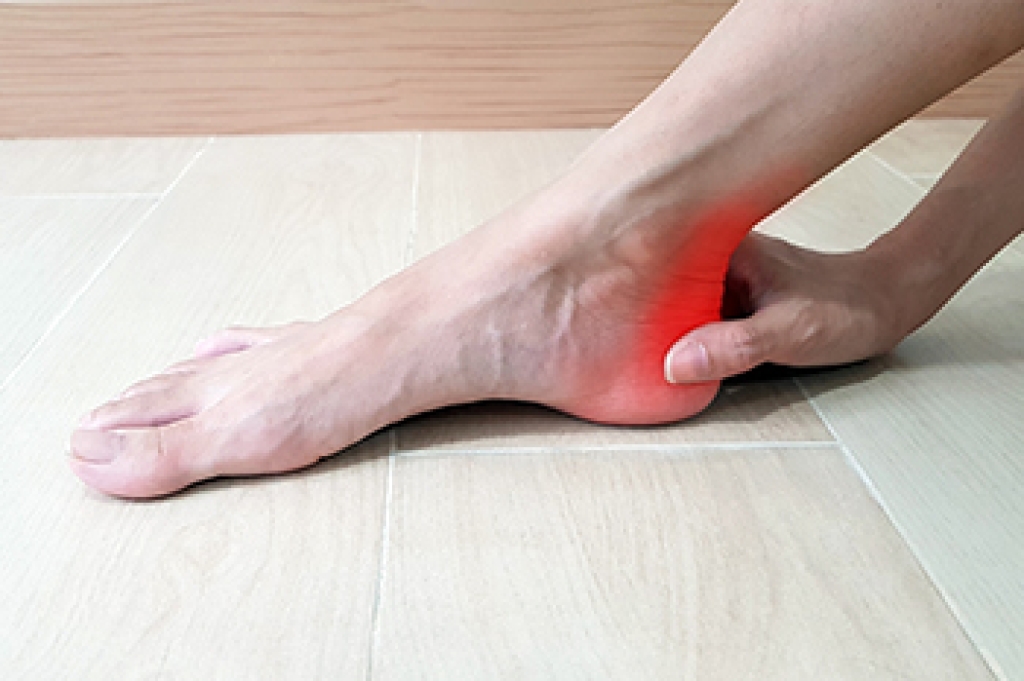
Achilles tendon pain often develops when the thick tendon connecting the calf muscles to the heel becomes irritated or inflamed from overuse, strain, or injury. This condition may cause aching, stiffness, or burning pain along the back of the heel or lower leg. This often happens after exercise or first getting out of bed in the morning. The area may appear swollen or thickened and can feel tender when touched. Running, climbing stairs, or prolonged walking may increase discomfort and make movement more difficult. Common causes include sudden increases in activity, tight calf muscles, wearing improper footwear, and repeated stress on the tendon. A podiatrist can evaluate the severity of the condition and determine whether there is inflammation, small tears, or tendon degeneration. Treatment may include wearing supportive footwear, targeted exercises, and activity modification. If you have Achilles tendon pain, it is suggested that you schedule an appointment with a podiatrist for an accurate diagnose and appropriate treatment plan.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Stephen Boykins, DPM of SoCal Podiatry, P.C.. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in Downey and Moreno Valley, CA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Warming Up the Ankles With Stretches

Warming up the ankles before activity helps prepare the joints and muscles for movement and reduces strain during exercise. The ankle is a weight-bearing joint that must move smoothly in several directions to support walking, running, and jumping. Simple stretches that point the toes away and toward the body can improve flexibility and range of motion. Gentle ankle circles and controlled inward and outward movements help loosen the ligaments and tendons that guide the joint. Ankle warm-up exercises improve balance and coordination, which can lower the risk of sprains and injuries. A podiatrist can evaluate ankle movement, check for stiffness or weakness, and order imaging to look for hidden problems. Treatment plans include guided stretching programs, supportive bracing and custom orthotics to improve alignment and protect the joint. If you have stiff or painful ankles, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and appropriate treatment.
Exercising your feet regularly with the proper foot wear is a great way to prevent injuries and build strength. If you have any concerns about your feet, contact Stephen Boykins, DPM from SoCal Podiatry, P.C.. Our doctor can provide the care you need to keep you pain-free and on your feet.
Exercise for Your Feet
Exercise for your feet can help you gain strength, mobility and flexibility in your feet. They say that strengthening your feet can be just as rewarding as strengthening another part of the body. Your feet are very important, and we often forget about them in our daily tasks. But it is because of our feet that are we able to get going and do what we need to. For those of us fortunate enough to not have any foot problems, it is an important gesture to take care of them to ensure good health in the long run.
Some foot health exercises can include ankle pumps, tip-toeing, toe rises, lifting off the floor doing reps and sets, and flexing the toes. It is best to speak with Our doctor to determine an appropriate regimen for your needs. Everyone’s needs and bodies are different, and the activities required to maintain strength in the feet vary from individual to individual.
Once you get into a routine of doing regular exercise, you may notice a difference in your feet and how strong they may become.
If you have any questions, please feel free to contact our offices located in Downey and Moreno Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How Diabetes Affects Foot Health
Diabetes can lead to serious foot problems by affecting circulation and nerve function. Reduced blood flow may slow healing, while peripheral neuropathy can cause numbness, making it difficult to feel injuries. This increases the risk of unnoticed cuts, ulcers, and infections. Risk factors include poor blood sugar control, long-term diabetes, and improper footwear. Daily foot checks and proper foot hygiene are essential for prevention. A podiatrist can monitor changes, treat wounds early, and provide guidance on protective footwear. If you have diabetes and notice changes in your feet, it is strongly suggested that you are under the care of a podiatrist who can help you to manage this serious condition.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Stephen Boykins, DPM from SoCal Podiatry, P.C.. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions, please feel free to contact our offices located in Downey and Moreno Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blog Archives
- 2026
- 2025
- 2024
- 2023
- 2022
- 2021