Connect With Us
Blog
Items filtered by date: December 2021
Gout Pain Can Be Managed
What Are Hammertoes?
Hammertoes are painful deformities that frequently form on the second, third, or fourth toe. The condition is often caused by an issue in foot mechanics. This can be caused by the person’s specific gait or the manner in which they walk, or by shoes that do not comfortably fit the deformity. Hammertoes can be formed after wearing shoes that are too narrow or short for the foot or have excessively high heels. Shoes that are not properly sized will force the toes into a bent position for long periods of time. This can cause the muscles to shorten and toes to bend into the deformity of a hammertoe.
Hammertoe can also be caused by complications from rheumatoid arthritis, osteoarthritis, trauma to the foot, heredity, or a cerebral vascular accident. Pain and difficult mobility of the toes, deformities, calluses, and corns are all symptoms of a hammertoe.
Someone who suspects they have the symptoms of a hammertoe should consult with a physician—particularly a podiatrist. Podiatrists diagnose and treat complications of the foot and ankle. If the podiatrist discovers that the affected toes are still flexible, treatment for the hammertoe may simply involve exercise, physical therapy, and better-fitting shoes. Treatment for hammertoes typically involves controlling foot mechanics, such as walking, through the use of customized orthotics.
For more serious cases in which the toes have become inflexible and rigid, surgery may be suggested. During the operation, the toe would receive an incision to relieve pressure on the tendons. A re-alignment of the tendons may then be performed by removing small pieces of bone to straighten the toe. In some cases, the insertion of pins is needed to keep the bones in the proper position as the toe heals. The patient is usually allowed to return home on the same day as the surgery.
If surgery is performed to repair a hammertoe, following the postoperative directions of your doctor is essential. Directions may include several stretches, picking up marbles with your toes, or attempting to crumple a towel placed flat against your feet. Wear shoes that have low heels and a wide amount of toe space to maintain comfort. Closed-toe shoes and high heels should be avoided. Shoes with laces allow the wearer to adjust how fitted he or she may want the shoes to be and also allow for greater comfort. To provide adequate space for your toes, select shoes that have a minimum of one-half inch of space between the tip of your longest toe and the inside of the shoe. This will also relieve pressure on your toes and prevent future hammertoes from forming.
Other preventative measures that can be taken include going shopping for new shoes in the middle of the day. Your feet are its smallest in the morning and swell as the day progresses. Trying on and purchasing new shoes midday will give you the most reliable size. Be sure to check that the shoes you purchase are both the same size. If possible, ask the store to stretch out the shoes at its painful points to allow for optimum comfort.
How Footwear Affects Hammertoe

To maintain healthy, strong feet, it is imperative to be familiar with common foot conditions, their causes, and how to prevent them. One troubling foot affliction that could threaten the vitality of your feet is called hammertoe, which has a notable causal relationship with certain kinds of footwear. Hammertoe affects the second, third, or fourth toe, occurring when an imbalance in the muscles around the toe’s middle joint causes the toe to stick up at the affected joint. This causes the toe to resemble a hammer. The condition, if left untreated, can make it especially difficult or painful to walk. Importantly, your choice of footwear can impact your likelihood of developing hammertoe. For example, shoes with small toe boxes that leave little room for the toes to sit comfortably in the shoe can force the toes into tight, twisted contortions. These contortions tighten the muscles in your toes, making hammertoe more likely. Additionally, high-heeled shoes can force your toes into tight, uncomfortable positions that might also tighten your muscles in the toes. To decrease your chances of developing a hammertoe, you might choose lower-heeled shoes with spacious toe boxes. If you think you have hammertoe or want to learn more about ways to prevent this condition, reach out to a podiatrist.
Hammertoe
Hammertoes can be a painful condition to live with. For more information, contact Stephen Boykins, DPM from SoCal Podiatry, P.C.. Our doctor will answer any of your foot- and ankle-related questions.
Hammertoe is a foot deformity that affects the joints of the second, third, fourth, or fifth toes of your feet. It is a painful foot condition in which these toes curl and arch up, which can often lead to pain when wearing footwear.
Symptoms
- Pain in the affected toes
- Development of corns or calluses due to friction
- Inflammation
- Redness
- Contracture of the toes
Causes
Genetics – People who are genetically predisposed to hammertoe are often more susceptible
Arthritis – Because arthritis affects the joints in your toes, further deformities stemming from arthritis can occur
Trauma – Direct trauma to the toes could potentially lead to hammertoe
Ill-fitting shoes – Undue pressure on the front of the toes from ill-fitting shoes can potentially lead to the development of hammertoe
Treatment
Orthotics – Custom made inserts can be used to help relieve pressure placed on the toes and therefore relieve some of the pain associated with it
Medications – Oral medications such as anti-inflammatories or NSAIDs could be used to treat the pain and inflammation hammertoes causes. Injections of corticosteroids are also sometimes used
Surgery – In more severe cases where the hammertoes have become more rigid, foot surgery is a potential option
If you have any questions please contact our offices located in Downey and Moreno Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ingrown Toenails
An ingrown toenail is a nail that has curved downward and grown into the skin. This typically occurs at either the nail borders or the sides of the nail. As a result, pain, redness, swelling, and warmth may occur in the toe. If a break in the skin forms due to the ingrown nail, bacteria may enter and cause an infection in the area; this is typically characterized by a foul odor and drainage.
Ingrown toenails have multiple reasons for developing. In many instances, the condition is a result of genetics and is inherited. The most common cause, however, is improper trimming; cutting the toenails too short forces the skin beside the nail to fold over. An ingrown toenail can also develop due to trauma, such as stubbing the toe, having an object fall on the toe, or participating in activities that involve repeated kicking or running. Wearing shoes that are too tight or too short can also cause ingrown toenails.
Treatment for an ingrown toenail varies between patients and the severity of the condition. In most cases, it is best to see your podiatrist for thorough and proper treatment. After examining your toe, your podiatrist may prescribe oral antibiotics to clear the infection if one is present. Surgical removal of either a portion of the nail or the entire nail may also be considered. In some cases, complete removal or destruction of the nail root may be required. Most patients who undergo nail surgery experience minimal pain afterward and can return to normal activity the following day.
Ingrown toenails can be prevented with proper nail trimming and by avoiding improper-fitting shoes. When cutting the toenails, be sure that you are cutting in a straight line and avoid cutting them too short. Shoes should not be too short or tight in the toe box.
When an Ingrown Toenail Becomes Dangerous
I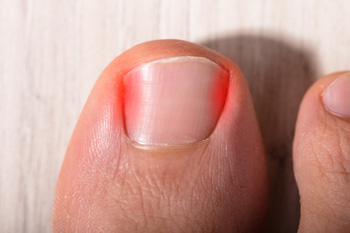 ngrown toenails can occur in individuals of all ages when the side of the nail digs into the skin. This condition is most prevalent in one’s big toe and will cause pain, discomfort, and redness where the ingrown nail meets the skin. Although the causes of ingrown toenails are varied, this condition frequently occurs due to improper nail care. If a toenail is cut too short, for example, the skin on the side of the nail can grow over top of the nail, eventually making it ingrown. Ingrown toenails can also develop when a toenail completely falls off following a serious foot injury or when the nail is severely ripped or misshapen. Some ingrown toenails—notably, milder ones—do not require immediate medical attention. However, making yourself aware of ingrown toenails is important to maintaining healthy feet because this condition can quickly become dangerous. Ingrown toenails may sometimes become infected, producing pus, swelling, warmness, and even unpleasant odors where the ingrown nail meets the skin. Letting such an infection go untreated may exacerbate the condition and the pain felt in the toenail. Upon receiving proper medical attention, your ingrown nail may be cared for by draining pus or removing sections of the ingrown nail. It is suggested you consult with your podiatrist if you feel an ingrown toenail is getting serious.
ngrown toenails can occur in individuals of all ages when the side of the nail digs into the skin. This condition is most prevalent in one’s big toe and will cause pain, discomfort, and redness where the ingrown nail meets the skin. Although the causes of ingrown toenails are varied, this condition frequently occurs due to improper nail care. If a toenail is cut too short, for example, the skin on the side of the nail can grow over top of the nail, eventually making it ingrown. Ingrown toenails can also develop when a toenail completely falls off following a serious foot injury or when the nail is severely ripped or misshapen. Some ingrown toenails—notably, milder ones—do not require immediate medical attention. However, making yourself aware of ingrown toenails is important to maintaining healthy feet because this condition can quickly become dangerous. Ingrown toenails may sometimes become infected, producing pus, swelling, warmness, and even unpleasant odors where the ingrown nail meets the skin. Letting such an infection go untreated may exacerbate the condition and the pain felt in the toenail. Upon receiving proper medical attention, your ingrown nail may be cared for by draining pus or removing sections of the ingrown nail. It is suggested you consult with your podiatrist if you feel an ingrown toenail is getting serious.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact Stephen Boykins, DPM of SoCal Podiatry, P.C.. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact our offices located in Downey and Moreno Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
All About Plantar Warts
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see the fleshy wart. A podiatrist should only be consulted if there is an excessive amount of pain. Plantar warts are not cancerous or dangerous, but they can affect your walking and continually reappear. Anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin to make tiny blood clots visible and examine the inside of warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. Although plantar warts usually do not require an excessive amount of treatment, there are ways to go about removing them. A common method is to freeze them off using liquid nitrogen, removing them using an electrical tool, or burning them off via laser treatment. For a less invasive treatment option, topical creams can be used through a doctor’s prescription. This treatment method takes more time, however. Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places. Avoid this especially if you have open sores or cuts on your feet. It is also important to avoid direct contact with warts in general, as they are highly contagious.
Dealing With Plantar Warts

If you notice a flat hardened callus on the bottom of your foot with tiny black spots showing beneath the skin, you may have a plantar wart. The area might be tender, but try not to touch it. This growth may be caused by the human papillomavirus (HPV), which is highly contagious and can enter your body through cuts or sores. The most common places to come into contact with HPV are swimming pools, locker rooms, and bathroom floors, all areas in which you are more likely to walk barefooted. Generally speaking, plantar warts are not dangerous, but they do spread rapidly. The most effective preventative method is to wear foot coverings in places where the virus thrives. If plantar warts become a common occurrence, refuse to go away on their own, or inhibit your ability to walk, it is a good idea to visit a podiatrist for guidance and a range of treatment options.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Stephen Boykins, DPM from SoCal Podiatry, P.C.. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our offices located in Downey and Moreno Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How to Care for Your Arthritic Foot
Arthritis is an inflammation of the joints and it can occur at any joint in the body, especially in the foot. It generally effects those who are older, however, it can occur at any age. Although there are many different forms of arthritis, there are three main types that occur in the foot. The three types are osteoarthritis, rheumatoid arthritis, and gout.
The primary cause of osteoarthritis is aging. As you age, cartilage degenerates around the joints which causes friction and pain. Obesity can cause osteoarthritis through mechanical stress. Injuries that damage joints can increase the probability as well. Finally, a family history of osteoarthritis can also increase chances of having it.
Rheumatoid arthritis occurs when the immune system attacks the joint linings and weakens them over a long time. While there is no known cause of rheumatoid arthritis, obesity and smoking can increase your chances of getting it. Women are also more likely to get it than men.
Gout is a form of arthritis that occurs when there is too much uric acid in your blood and painful crystals form in your joints. Men are more likely to have gout than women. People who are obese or drink alcohol often are also more likely to develop gout. Furthermore, having diabetes, heart disease, high blood pressure, high cholesterol, gastric bypass surgery or a family history of gout may increase your likelihood of developing the condition.
Symptoms of arthritis include pain, stiffness, swelling in the joints. These symptoms can make it harder and more painful to walk. Physical activity can increase pain and discomfort. Furthermore, joint pain can worsen throughout the day for osteoarthritis. Gout attacks generally last several days with the first few being the worst.
Diagnosis of gout includes either a joint fluid test or a blood test. X-ray imaging can detect osteoarthritis but not gout. On the other hand, there is no blood test for osteoarthritis. Rheumatoid arthritis is difficult to diagnosis. Doctors utilize family and personal medical history, a physical examination, and antibody blood tests to determine if you have rheumatoid arthritis.
Treatment varies for the different kinds of arthritis. Anti-inflammatory medication or steroids can help reduce pain from inflammation of the joints. Changing shoe types can help with some symptoms. Wider shoes can help with discomfort from gout and osteoarthritis. High heels should be avoided. Shoes with proper arch support and that take pressure off the ball of the foot can help with rheumatoid arthritis. Drinking lots of water can also help rid uric acid from the blood. Losing weight, improving your diet, and limiting alcohol and smoking can also help prevent or lessen the symptoms of arthritis.
If you are having trouble walking or pain in your feet, see a podiatrist to check if you have arthritis.
Arthritis Can Affect the Feet, Toes, and Ankles
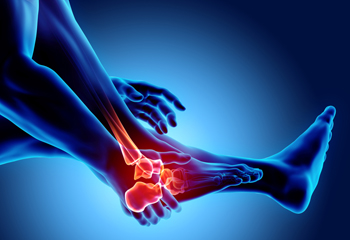
Arthritis can have painful effects on the feet, toes, and ankles. Some of the more common types of arthritis are described here. Osteoarthritis (OA) mainly affects the first metatarsal joint connecting the big toe to the foot, as well as the midfoot and ankle. It is a wear and tear arthritis because it causes cartilage in the joints to wear down, leading the bones to rub together. Rheumatoid arthritis (RA) is an autoimmune disease where the immune system attacks the lining of the joints, including the ankle, heels, midfoot, and forefoot. Over time, the damage can lead to joint deformity and/or disability. Gout is an inflammatory type of arthritis caused by uric acid build up and crystallization in joints, often in the big toe of the foot. Psoriatic arthritis (PsA) is also an inflammatory arthritis that can happen to those with psoriasis. It can affect the joints in the ankle as well as ligaments and tendons in the foot. Anyone with any type of arthritis can experience foot involvement, which can make it hard to walk and perform activities of daily life. While arthritis has no cure, treatment options exist to slow the progression of the disease and relieve symptoms. If you experience the pain of arthritis in your feet and ankles, seek the counsel of a podiatrist who can help you manage pain, stay active, and lead a fulfilling life.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Stephen Boykins, DPM from SoCal Podiatry, P.C.. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a term that is commonly used to describe joint pain. The condition itself can occur to anyone of any age, race, or gender, and there are over 100 types of it. Nevertheless, arthritis is more commonly found in women compared to men, and it is also more prevalent in those who are overweight. The causes of arthritis vary depending on which type of arthritis you have. Osteoarthritis for example, is often caused by injury, while rheumatoid arthritis is caused by a misdirected immune system.
Symptoms
- Swelling
- Pain
- Stiffness
- Decreased Range of Motion
Arthritic symptoms range in severity, and they may come and go. Some symptoms stay the same for several years but could potentially get worse with time. Severe cases of arthritis can prevent its sufferers from performing daily activities and make walking difficult.
Risk Factors
- Occupation – Occupations requiring repetitive knee movements have been linked to osteoarthritis
- Obesity – Excess weight can contribute to osteoarthritis development
- Infection – Microbial agents can infect the joints and trigger arthritis
- Joint Injuries – Damage to joints may lead to osteoarthritis
- Age – Risk increases with age
- Gender –Most types are more common in women
- Genetics – Arthritis can be hereditary
If you suspect your arthritis is affecting your feet, it is crucial that you see a podiatrist immediately. Your doctor will be able to address your specific case and help you decide which treatment method is best for you.
If you have any questions, please feel free to contact our offices located in Downey and Moreno Valley, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.